In the fourth of our weekly series of articles by NUI Galway researchers, Dr. Kieran Ryan, VISICORT Project Manager, writes about ‘Vision‘ and VISICORT’s research into improving corneal transplant outcomes by preventing rejection.

Eyes are the organs of vision, detecting light and converting it into electro-chemical impulses in neurons. Eyes come in ten different forms, with the simplest types of ‘eyes’, merely eyespots, detecting whether the immediate surroundings are light or dark (photoreception).
Photoreception is known to have evolved a long time ago in single-celled organisms. The advantage of improved vision in food gathering, escape from predators and even finding a mate, would have driven the evolution of vision to also detect movement, colour and form. Most of the improvements in early eyes are believed to have taken only a few million years to develop. Based on shared genetic sequences, it is now widely accepted that 540 million years ago, a single, common origin for all eyes in higher animals arose. These “proto-eyes” are thought to have developed in predators first, giving them a distinct advantage over their prey and other competing predators.

Eyes can be classified into ‘simple eyes’, with one concave photoreceptive surface, and ‘compound eyes’, where a number of individual lenses are laid out on a convex surface. The majority of animal species possess complex optical systems, which collect light from their environment and convert it into electrical signals for processing into an image by the brain. Although classified as a ‘simple eye’, the human eye is an intricate organ, made up of a number of components, each with their role to play in collecting, focusing, converting and processing light
The cornea is the transparent front part of the eye that covers: (i) the iris – the pigmented part of the eye which gives it its colour, and is so called because in Greek mythology, ‘Iris’ was the goddess of the rainbow; (ii) the pupil – the part of the eye which narrows or widens to control the amount of light entering, and which appears black as the light is absorbed; and (iii) the aqueous humour-filled anterior chamber, through which light passes on the way to the lens.
As well as protecting the front parts of the eye, the cornea focuses incoming light, providing two-thirds of the eye’s optical power. Thus, any damage to the cornea, through trauma, infection, and other diseases, can have devastating effects on an individual’s eyesight, and is the fourth most common cause of blindness, affecting 10 million people worldwide.
Corneal transplantation is the most frequently performed transplant procedure in humans, with over 100,000 procedures each year worldwide. It is often the only treatment available to restore sight to people who have lost vision due to diseases of the cornea.

However, despite advances in microsurgery and immunosuppressive treatments, the transplanted cornea is rejected in about 30% of patients who undergo transplantation, due to an adverse immune response. Treatment with corticosteroids is currently the most successful way of combating corneal rejection, although it is frequently ineffective in some patients.
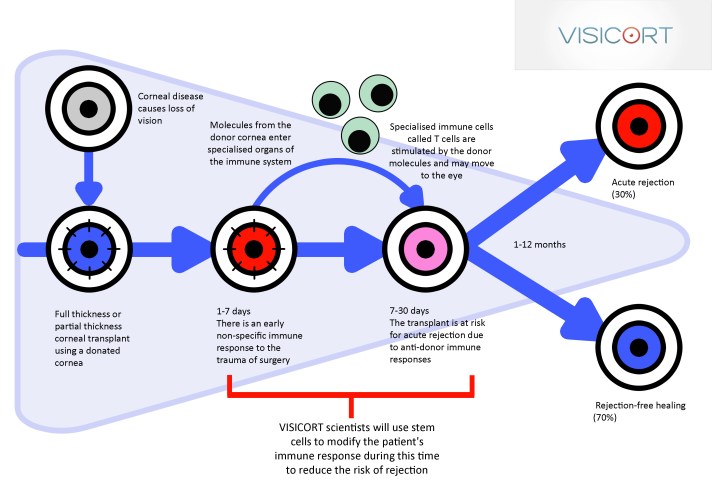
Researchers at the NUI Galway Regenerative Medicine Institute (REMEDI) have come together with NUI Galway spin-out company Orbsen Therapeutics, and the Centre for Cell Manufacturing Ireland (CCMI), to lead a €6M EU Framework Programme 7-funded project aimed at better understanding the immune responses to corneal transplants. The researchers also aim to improve corneal transplant outcomes using a stem cell therapy to modify the immune response in high risk transplant patients.
Known as “VISICORT” (Adverse Immune Responses and their Prevention in Corneal Transplantation), the five year project is being jointly coordinated by Professor Matthew Griffin and Dr Thomas Ritter, in partnership with 11 other academic and industry-based partners from France, Germany, Denmark and the UK.
The Galway teams will build on an existing model system, which shows that stem cells can have a positive effect on the immune system during transplantation, leading to an improvement in the overall success of corneal transplantation. The final year of the project will involve a clinical trial, testing the usefulness of stem cells in corneal transplant, using cells manufactured at NUI Galway in the CCMI.
To learn more about this ongoing project, you can watch Dr. Ritter and his team on the RTE’s Six One News (scroll to 16:48) or speaking on RTE’s Morning Ireland radio programme (scroll to 1:27:52).
VISICORT is a supporter of the ReelLIFE SCIENCE schools science competition.


